 An orotracheal tube was placed, the anesthesia machine was connected for manual and mechanical ventilation and a cardiac massage was started alternating 30 compressions and 2 ventilations. The Code Blue/5 link was immediately activated and basic and advanced life support was initiated. The clinical examination revealed an unconscious, cyanotic patient, pulseless and with dilated and fixed pupils. The patient was immediately placed on a stretcher in the OR. The patient experienced a cardiac arrest just when he was about to start a surgical procedure in the OR. The case is of a 63-year-old patient, facial plastic surgeon, with a relevant cardiovascular history: 1 – Aortic valve replacement with mechanical prosthesis performed 10 years ago because of aortic insufficiency 2 – Anticoagulation with warfarin 3 – Pacemaker because of a third degree AV block as a result of valve surgery 4 – HBP treated with metoprolol 25 mg-day 5 – Dislipidemia and undergoing statin treatment. Luego de la búsqueda bibliográfica en las bases de datos médicas electrónicas de: Medline, Lilacs, Scielo y Ovid, se discuten en esta revisión narrativa algunos aspectos interesantes reportados por otros autores en relación con este tema. A los 3 meses del evento el paciente se encuentra reintegrado a la vida familiar, social y laboral en perfectas condiciones. A las 18 h el paciente despierta sin daño neurológico evidente, permanece en la UCI por un mes, resolviendo los problemas relacionados con el síndrome isquemia-reperfusión, y luego de 20 días más con fisioterapia en la habitación, el paciente es dado de alta con recomendaciones de rehabilitación en el hogar sin ningún déficit neurológico. Tras otra descarga y más amiodarona, el paciente recupera la circulación espontánea, se normalizan los signos vitales y se deja en la UCI en condicio-nes hemodinámicamente estables. La reanimación se mantiene constante durante todo el proceso, que dura 1 h y 45 min, incluyendo el traslado a una clínica de tercer nivel, en donde consideran que el paciente está en asistolia. El paciente alterna entre fibrilación ventricular, actividad eléctrica sin pulso y asistolia. Se inician maniobras de reanimación básica y avanzada, se evidencia fibrilación ventricular y se desfibrila en 4 oportunidades sin éxito, se aplican epinefrina, bicarbonato, amiodarona y lidocaína. Se reporta el caso de un paciente de 63 años de edad, cirujano plástico facial de profesión, con antecedentes cardiovasculares de reemplazo valvular aórtico, hipertensión arterial, marca-pasos y anticoagulación, quien presenta muerte súbita de origen cardíaco en salas de cirugía. 
This narrative discussion considers some interesting aspects reported by other authors on the topic, based on a bibliography search in Medline, Lilacs, Scielo, and Ovid. Three months later, the patient is doing perfectly well and leading an active family, social and labor life. After 20 more days of physical therapy in his hospital room, the patient was discharged with no neurological deficit and a recommendation for home-based rehabilitation. After 18 h, the patient woke up with no evident neurological damage and remained in the ICU for one month for treatment of the ischemic-reperfusion syndrome. Following an additional discharge and amiodarone, the patient recovered spontaneous circulation the vital signs were normalized and the patient remained in the ICU under hemodynamically stable conditions. Resuscitation was maintained throughout the process which lasted one hour and 45 min, including transfer to a third level clinic where the patient was considered to be asystolic. The patient alternated between ventricular fibrillation, pulseless electrical activity and asystole. Epinephrine, bicarbonate, amiodarone and lidocaine were administered. 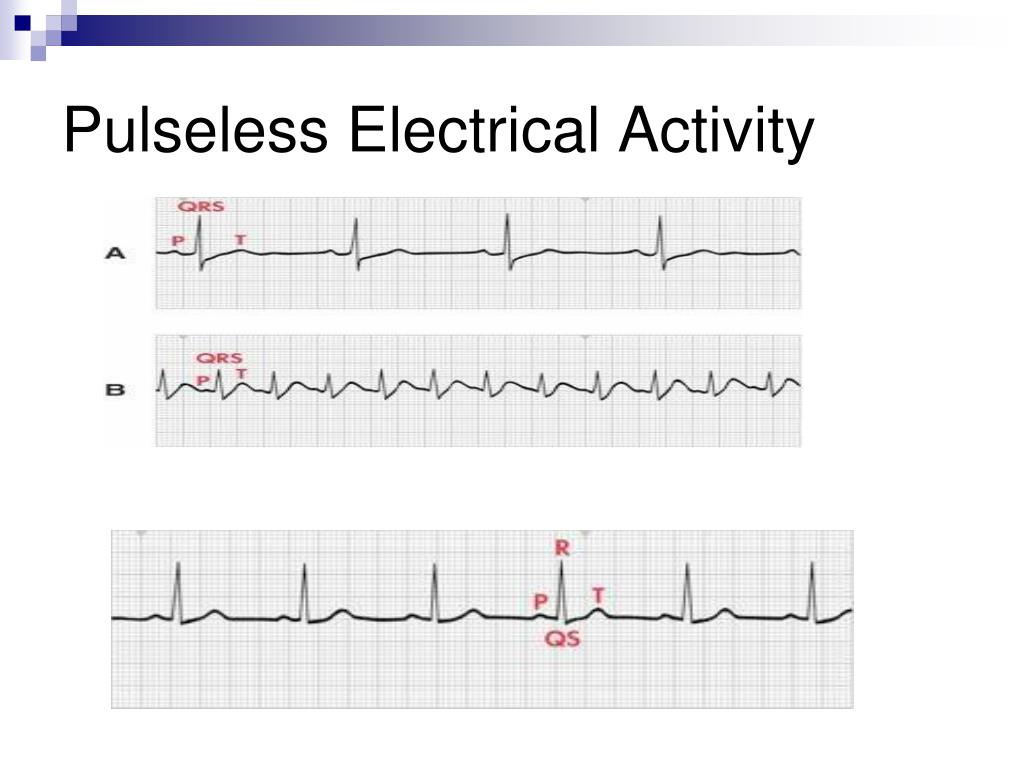
Basic and advanced life support maneuvers were initiated there was evidence of ventricular fibrillation and the patient was defibrillated 4 times unsuccessfully. This is the case of a 63-year-old patient, who is a plastic surgeon and has a history of aortic valve replacement, hypertension, pacemaker and anticoagulation, who experienced cardiac sudden death in the OR. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
